Medication safety represents an important challenge in children. There are limited studies on medication errors in pediatric patients visiting emergency departments. To help bridge this gap, we characterized the medication errors detected in these patients, determining their severity, the stages of the medication process in which they occurred, the drugs involved, and the types and causes associated with the errors.
MethodsWe conducted a multicenter prospective observational study in the pediatric emergency departments of 8 Spanish public hospitals over a 4-month period. Medication errors detected by emergency pediatricians in patients between 0 and 16 years of age were evaluated by a clinical pharmacist and a pediatrician. Each medication error was analyzed according to the updated Spanish Taxonomy of Medication Errors.
ResultsIn 99,797 visits to pediatric emergency departments, 218 (0.2%) medication errors were detected, of which 74 (33.9%) resulted in harm (adverse drug events). Preschoolers were the age group with the most medication errors (126/218). Errors originated mainly in the prescribing stage (66.1%), and also by self-medication (16.5%) and due to wrong administration of the medication by family members (15.6%). Dosing errors (51.4%) and wrong/improper drugs (46.8%) were the most frequent error types. Anti-infective drugs (63.5%) were the most common drugs implicated in medication errors with harm. Underlying causes associated with a higher proportion of medication errors were “medication knowledge deficit” (63.8%), “deviation from procedures/guidelines” (48.6%) and “lack of patient information” (30.3%).
ConclusionsMedication errors presented by children attending emergency departments arise from prescriptions, self-medicationand administration, and lead to patient harm in one third of cases. Developing effective interventions based on the types of errors and the underlying causes identified will improve patient safety.
La seguridad de medicamentos en pediatría supone un verdadero reto. Se dispone de escasos estudios que hayan analizado los errores de medicación en los pacientes pediátricos que acuden a los servicios de urgencias. El objetivo de este estudio ha sido caracterizar los errores detectados en estos pacientes, determinando su severidad, los procesos afectados, los medicamentos implicados, y los tipos de errores y causas asociados.
MétodosEstudio multicéntrico observacional prospectivo realizado en los servicios de urgencias de 8 hospitales públicos españoles durante 4 meses. Los errores de medicación detectados por los pediatras de urgencias en pacientes entre 0 y 16 años fueron evaluados por un farmacéutico y un pediatra. Los errores de medicación fueron analizados utilizando la Taxonomía Española de Errores de Medicación actualizada.
ResultadosEn 99.797 visitas a urgencias se detectaron 218 (0,2%) errores de medicación, de los cuales 74 (33,9%) causaron daños (eventos adversos por medicamentos). Los preescolares fueron el grupo poblacional con mayor número de errores de medicación (126/218). Los errores se originaron mayoritariamente en la prescripción (66,1%), por automedicación (16,5%) y por administración equivocada por parte de familiares (15,6%). Los tipos de errores más frecuentes fueron “dosis incorrectas” (51,4%) y “medicamento inapropiado” (46,8%). Los antiinfecciosos (63,5%) fueron los fármacos más comúnmente implicados en los errores con daño. Las causas subyacentes asociadas a una mayor proporción de errores de medicación fueron: “falta de conocimiento del medicamento” (63,8%), “falta de seguimiento de los procedimientos” (48,6%) y “falta de información del paciente” (30,3%).
ConclusionesLos errores de medicación en la población pediátrica que acude a urgencias se producen en la prescripción, por automedicación y en la administración, provocando daños a los pacientes en un tercio de las ocasiones. Desarrollar prácticas seguras basadas en los tipos de errores detectados y sus causas subyacentes, mejorará la seguridad de los pacientes.
The safe use of medications represents one of the major challenges for the pediatric population, as they are more likely than adults to experience medication errors (MEs), and these errors are more frequently harmful.1 Several factors contribute to the increased risk of medication incidents in children, including the need for carrying out multiple calculations to individualize doses based on patient age and/or body weight, the lack of appropriate pediatric formulations, the need to use unlicensed or off-label medicines, and the lack of adequate dosing information for children.2 MEs in pediatric patients occur in all healthcare settings, though incidence appears to be higher in neonatal units, pediatric intensive care units, and emergency rooms.2–4 These errors take place in all processes of the medication use system, though they appear to be more frequent in prescription and administration, including home administration to patients by parents or caregivers.3–5
The World Health Organization (WHO) launched its third Global Patient Safety Challenge: Medication Without Harm, with the goal of reducing severe avoidable medication-related harm that is associated with MEs by 50% within five years.6 This safety challenge has been incorporated into the Global Patient Safety Action Plan 2021–2030.7 The WHO considers children as patients at a high-risk of experiencing MEs with severe clinical outcomes and has established a priority to take action to reduce MEs in this population.8 To achieve the goal of this WHO challenge, a deep understanding of the nature of MEs in children will be important for developing effective interventions.
Emergency departments (EDs) provide key settings for detecting and gathering valuable information about incidents caused by medications, as they are an interface between hospitals and communities.9 Numerous studies have been carried out on medication incidents among the pediatric population who presented at EDs.10–15 However, most of these studies were retrospective and were focused on identifying adverse drug events (ADEs) and determining the incidence, which ranged from 0.2% and 8.0%, as well as their severity and the medications implicated. Only a few studies analyzed ADEs preventability, which ranged from 20.3% to 66.7%, and provided any information about the MEs associated with these preventable ADEs.10,13–15 They also failed to analyze MEs that did not result in harm. However, it is undoubtedly critically important to identify and analyze all MEs that occur among the pediatric population in order to establish safe medication practices.
This study was conceived to help bridge this gap. Its main objective was to prospectively identify and chraracterize the MEs that occur among pediatric patients visiting EDs, determining their severity, the stages of the medication process in which they occurred, the drugs involved, and the types and causes associated with the errors.
MethodsThis study is part of a larger research project carried out to determine the incidence and to characterize all types of medication-related incidents in patients visiting pediatric EDs.16 It was a multicenter prospective observational study that was conducted in the pediatric ED of 8 Spanish public hospitals over a 4-month period (March 1st to June 30th, 2017). The study protocol was authorized by the ethics committee at each participating hospital, according to Spanish regulations.
We studied all patients <16 years old who visited the EDs of the hospitals. The primary variable in our study was ME experienced by the patients regardless of whether or not the incident were the reason they visited the EDs. It was defined as “any avoidable event that may cause or lead to inappropriate medication use or patient harm while the medication is under the control of the healthcare professional, patient or consumer”.17 MEs were classified into two groups: MEs either resulting in harm (or preventable ADEs) or not resulting in harm.
We began by developing an instruction manual that was explained in detail at a meeting at each hospital with all coordinators, who were clinical pharmacists. Several training exercises were also reviewed so that these researchers would have a chance to look at real cases in order to clear up any doubts regarding the methods and evaluation. Additionally, at every hospital there was a pediatrician assigned as responsible for the study.
At each hospital, a decision-making algorithm to help identify medication incidents eligible for the study, and a series of instructions on how to obtain the most relevant information about the errors during the interview with the patients' parents or caregivers were distributed among the staff at each pediatric ED. Authorization was requested from parents or caregivers to include information regarding their child's treatment in the study, through the informed consent document.
They were required to gather a minimum amount of data on a checklist to make the subsequent analysis possible. The clinical pharmacist at each hospital visited the emergency room to collect these checklists, and complete all the additional information required to properly characterize the MEs. To do that, they reviewed the ED's admission reports, the current and previous months' laboratory reports, and the medical prescriptions issued on discharge from hospital and from primary care.
The following variables were recorded for each medication error: sex, weight, date of birth, age group (5 groups were defined: neonates -from birth to 28 days-, infants -from 1 to 12 months-, preschoolers –from 1 to 5 years-, schoolers –between 6 and 12 years- and adolescents – from 13 to 16 years), allergies, reason for consultation, and patients' pharmacological treatment (brand name, generic name, strength and dosage form, dose, frequency and route of administration, duration of treatment, indication, and prescriptor).
The clinical pharmacist and the pediatrician responsible at each hospital evaluated the errors that were detected. Severity was determined using the National Coordinating Council for Medication Error and Prevention (NCCMERP) Index.18 Preventability was evaluated using Schumock & Thornton's preventability criteria adapted by our working group.19 Whenever questions or discrepancies arose, the attending pediatrician was contacted. In addition, each medication error was analyzed according to the updated Spanish Taxonomy of Medication Errors established by Otero et al.,20 which is an adaptation of the NCCMERP. Errors were characterized according to the personnel involved, the stage in the medication use process in which they occurred, type of errors, and possible associated causes. This taxonomy includes an error type called “self-medication” to typify errors caused from the administration of inappropriate medication on the initiative of the patient's own family or caregivers.
Once completed, the data were introduced into a web-based medication-related error registration platform specifically developed for the Spanish Institute for Safe Medication Practices (ISMP-Spain) for the study. The principal investigator reviewed and validated the data for consistency. All questions were directed to the coordinator at each hospital for resolution.
A descriptive statistical analysis was carried out of the characteristics of the subjects with respect to the explanatory variables considered in the study. The analyses included frequency distributions for qualitative variables. The statistical analysis was carried out using the SPSS® 2.0 software package.
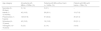
ResultsOver the study period, there were 99,797 visits to the pediatric EDs and 218 MEs detected in 218 patients. This gives an incidence of 0.2% of patients with a medication error. Of these, 54.6% were male. The average age was 45.6 ± 42.5 months. Of the total number of errors recorded, 74 (33.9%) caused harm to patients. A total of 10.6% of the patients required hospitalization or observation in emergency room beds. Preschoolers were the age group in which MEs were most frequently detected (57.8%) (Table 1). In both schoolers and teenagers more errors were found that caused harm than without harm.
Medication errors by age category.
| Age category | All patients with MEsn = 218No. (%) | Patients with MEs without harm n = 144No. (%) | Patients with MEs with harmn = 74No. (%) |
|---|---|---|---|
| Neonates (0–28 days) | 3 (1.4) | 3 (2.1) | – |
| Infants (1–12 months) | 42 (19.3) | 29 (20.1) | 13 (17.6) |
| Preschoolers (1–5 years) | 126 (57.8) | 91 (63.2) | 35 (47.3) |
| Schoolers (6–12 years) | 42 (19.3) | 19 (13.2) | 23 (31.1) |
| Teenagers (13–16 years) | 5 (2.3) | 2 (1.4) | 3 (4.0) |
MEs: Medication errors.
A high number of MEs that did not cause harm to patients were of category C (121/144; 84.0%). On the other hand, the majority of errors that caused harm were of category E (67/74; 90.5%) (Table 2). Prescription errors were the most frequent, occurring in 66.1% of the total errors (144/218) and in 67.6% of errors with harm (50/74). Of these prescription errors, 45.9% originated principally at pediatric physicians offices and at emergency rooms in primary care centers and only 7.4% at specialized care centers. Other errors were caused by self-medication (16.5%) and by medications being administered by family members or caregivers (15.6%). Of the 20 cases in which patient education was the initial stage when the error occurred, 17 led to a subsequent error in administration.
Categories of severity of the medication errors and stage of the medication use process where occurred.
| Stage a | All MEsn = 218No. (%)⁎ | MEs without harm | MEs with harm | ||||
|---|---|---|---|---|---|---|---|
| Totaln = 144No. (%)⁎ | Cn = 121No. | Dn = 23No. | Totaln = 74No. (%)⁎ | En = 67No. | Fn = 7No. | ||
| Prescribing | 144 (66.1) | 94 (65.3) | 83 | 11 | 50 (67.6) | 47 | 3 |
| Self-medication | 36 (16.5) | 28 (19.4) | 24 | 4 | 8 (10.8) | 7 | 1 |
| Administration by familiar or caregiver | 34 (15.6) | 20 (13.9) | 12 | 8 | 14 (18.9) | 11 | 3 |
| Patient education | 20 (9.2) | 8 (5.6) | 5 | 3 | 12 (16.2) | 10 | 2 |
| Others b | 4 (1.8) | 2 (1.4) | 2 | – | 2 (2.7) | 2 | – |
| TOTAL | 238 | 152 | 126 | 26 | 86 | 77 | 9 |
MEs: Medication errors; C: An error occurred that reached the patient, but did not cause harm; D: An error occurred that resulted in the need for increased patient monitoring, but no patient harm; E: An error occurred that resulted in need for treatment or intervention and caused temporary patient harm; F: An error occurred that resulted in initial or prolonged hospitalization and caused temporary patient harm.
After analysis, a total of 248 types of errors were considered associated with the 218 MEs detected (Table 3). The most frequent types of error were wrong dose (51.4%) and wrong/improper drug (46.8%). Also, the greatest percentage of errors with harm were related to a wrong dose (66.2%), especially subtherapeutic dosage, wrong/improper drug (29.7%) and drug/dose omission (13.5%). Taken all together, the MEs associated with the use of subtherapeutic doses, inappropriate drug according to the diagnosis, or drug/dose omission accounted for 66.3% of the errors with harm and resulted in therapeutic failure.
Type of errors associated with the medication errors detected.
| Type of medication error a | Total MEsn = 218No. (%)⁎ | MEs without harmn = 144No. (%)⁎ | MEs with harmn = 74No. (%)⁎ |
|---|---|---|---|
| Wrong dose | 112 (51.4) | 63 (43.7) | 49 (66.2) |
| - Underdosing | 67 (30.7) | 29 (20.1) | 38 (51.3) |
| - Overdosing | 45 (20.6) | 34 (23.7) | 11 (14.9) |
| Wrong/improper drug | 102 (46.8) | 80 (55.5) | 22 (29.7) |
| - Unnecessary medication | 62 (28.4) | 54 (37.5) | 8 (10.8) |
| - Inappropriate drug according to diagnosis | 25 (11.5) | 14 (9.7) | 11 (14.9) |
| - Inappropriate drug for the patient | 7 (3.2) | 5 (3.5) | 2 (2.7) |
| - Other | 8 (3.7) | 7 (4.9) | 1 (1.3) |
| Drug/ dose omission | 12 (5.5) | 2 (1.4) | 10 (13.5) |
| Wrong frequency | 9 (4.1) | 7 (4.9) | 2 (2.7) |
| Wrong method of preparation | 3 (1.4) | 3 (2.1) | – |
| Wrong route of administration | 3 (1.4) | 2 (1.4) | 1 (1.3) |
| Monitoring error | 2 (0.9) | – | 2 (2.7) |
| Wrong dosage form | 2 (0.9) | 2 (1.4) | – |
| Other types | 3 (1.4) | – | 3 (4.1) |
| TOTAL | 248 | 159 | 89 |
MEs: Medication errors.
The main class of drugs implicated in the MEs was anti-infective drugs (55.0%), principally penicillins (amoxicillin and its association with clavulanic acid), which was also the drug class most frequently related to the errors with harm (63.5%) (Table 4). It's important to note that the most frequent types of errors with anti-infective drugs were prescribing infra-therapeutic doses (51/120) (for example, a dose insufficient for treating an acute otitis media that had brought the patient to the ED because of a lack of improvement in symptoms). Also, prescribing an unnecessary medication (41/120), mostly for treating viral infections in the respiratory tract, or for selecting an inappropriate antibiotic for the diagnosis to be treated (17/120). On the other hand, the most common type of error with medications for the nervous system was the use of higher doses (24/33). Fifteen of these errors were caused by using an excessive dose of acetaminophen due to incorrect self-medication on the part of parents or caregivers, or administration errors due to misunderstanding the package insert.
Drugs involved in the medication errors according to the anatomical therapeutic chemical (ATC) classification system.
| ATC level 1 | Total MEsn = 218No (%)⁎ | MEs without harmn = 144No (%)⁎ | MEs with harmn = 74No (%)⁎ |
|---|---|---|---|
| J- Anti-infectives for systemic use | 120 (55.0) | 73 (50.7) | 47 (63.5) |
| R- Respiratory system | 34 (15.6) | 29 (20.1) | 5 (6.7) |
| N- Nervous system | 33 (15.1) | 23 (16.0) | 10 (13.5) |
| M- Musculoskeletal system | 19 (8.7) | 13 (9.0) | 6 (8.1) |
| H- Systemic hormonal preparations | 12 (5.5) | 8 (5.5) | 4 (5.4) |
| A- Alimentary tract and metabolism | 8 (3.7) | 5 (3.5) | 3 (4.1) |
| Others | 6 (2.8) | 3 (2.1) | 3 (4.1) |
| TOTAL | 232 | 154 | 78 |
MEs: Medication errors.
The underlying causes most commonly associated with prescription errors were “medication knowledge deficit” (63.8%) and “deviation from procedures/guidelines” (48.6%), and these causes were also most frequently related to errors with harm (73.0% and 55.4%, respectively). Another cause mainly attributed to administration errors was “inadequate communication of prescription” (28.4%), also frequently associated with errors with harm (32.4%).
DiscussionThis is the first prospective study carried out in Spain to explore the MEs presented by pediatric patients who attended EDs, whether or not the ME had been the reason for the ED visit. A total of 218 MEs were detected in 99,797 visits, which gives an incident rate of 0.2%, low in comparison to the studies that analyzed ADEs conducted in the same healthcare settings. This fact was attributed to Spanish EDs being understaffed and overworked.16
The age group for which the greatest number of MEs was detected were preschool children, a finding that agrees with that found in studies on ADEs in EDs,10–12 as well as in error notification systems and poison centers which have determined a higher incidence of errors among children under 4–5 years of age.2,5,21 However, it was the older children and adolescents who presented a higher proportion of MEs with harm. This finding also coincided with the epidemiologic study on ADEs carried out by Lombardi et al,15 who reported a greater incidence of serious ADEs in older children.
A large proportion of the errors originated during the prescription stage (66.1%), above all at pediatric primary care doctors offices. Also frequent were errors related to self-medication when drugs were administered in the homes of the patients and often associated with a lack of knowledge on the part of family members or caregivers. The higher frequency of errors during these stages has been pointed out in several publications,3,4,22,23 although studies on MEs among pediatric outpatients are really quite limited.
As far as the types of error, dosing errors were the leading error type we detected, not only in the total number of errors but also in the errors with harm. This is not surprising since one of the main risk factors for errors in pediatric patients is the need to individualize the dose according to age, weight, or body size as was mentioned earlier.2 Another contributing factor to dosing errors in the pediatric population is having to habitually use liquid oral formulations with dosing devices susceptible to these errors, making it especially important to explain to parents how they should use the device to administer the correct dose.24
Other types of error frequently found were those related to inappropriate medication prescription, due to being unnecessary or inappropriate for the disease or the patient. Few data about inappropriate prescriptions in pediatric patients have been published, though a recent study in France focused on describing trends in pediatric outpatient prescription at the population level and found several areas of inappropriate prescriptions, including antibiotics and systemic corticosteroids.25 In this sense, we should point out that the Choosing Wisely campaign initiated to reduce the use of unnecessary drugs includes statements from the American Academy of Pediatrics regarding conditions for which best evidence supports not providing certain treatment,26 for example, not using antibiotics for viral respiratory illnesses. Additionally, lists of drugs that are potentially inappropriate for prescribing in pediatric patients have been published in both Europe27 and the United States28 to improve the medication use safety in children, which shows clearly that inappropriate medication prescription is a recognized and serious concern for this population, though it has not been well dimensioned.
Antibiotics were the most common drug class causing MEs, just as with the findings of studies on ADEs in EDs.14,15 Additionally, the types of error that were most frequent were the use of subtherapeutic doses (as also reported in the prospective study by Zed et al.14) and the unnecessary prescription of antibiotics. A recent study carried out in Spain29 that analyzed the adequacy of antimicrobial stewardship at discharge from a pediatric ED, showed that in 50.7% of cases the antibiotics were inadequate due to an incorrect dose, unnecessary prescribing, or inappropriate selection. There was also a European study published that observed wide variation between European EDs in prescriptions of antibiotics in febrile children.30 Overall, one-third of prescriptions were inappropriate or inconclusive, with marked variation among EDs. All of these data demonstrate the need to implement antimicrobial stewardship guidelines across Europe in order to prevent the inadequate use of antibiotics and limit antimicrobial resistance.
The information obtained in this study on MEs in children and their possible causes may be of great value for prioritizing actions to improve medication use safety in this population. This study reveals that the problem is complex and requires multiple actions that will address the four domains that define the third WHO challenge: health care professionals, patients and the public, medicines and systems, and medication practices. Thus, the interventions should be fundamentally oriented towards prescribing physicians, reinforcing their knowledge of safe medication practices, promoting learning and following clinical practice guidelines, and insisting on the need to maintain appropriate communication about prescription decisions with parents and/or caregivers. They should also concentrate on parents and/or caregivers, providing them with adequate knowledge and making them participants in the treatment, and in the general population through education campaigns that manifest the seriousness of self-medication risks. In addition, clinical decision support tools that help in adjusting prescriptions to the characteristics of pediatric patients should be implemented.
This study has several limitations. The first is that many incidents may have not been reported as a result of the high workload of EDs, the high turnover of medical staff, and the unavailability of an onsite clinical pharmacist. Second, there is a certain degree of subjectivity in the analysis of the MEs, especially regarding causation, though researcher training was applied in an attempt to avoid it. Among the strong points of the study is that this is a prospective and multicenter study and that error evaluation was carried out by a multidisciplinary team, which provides for broader knowledge for analyzing the information and reducing the biases derived from a partial analysis perspective.
In summary, the MEs presented by children who visit EDs originate principally in prescription, self-medication, and in administering medications in homes, and lead to patient harm in a third of the cases. Developing effective interventions addressing the types of errors and the underlying causes identified will improve safety for these patients.
Authorship declarationAll authors declare that they have made a substantial contribution to the present manuscript. Each author has specifically been in charge of the following:
GC-B participated in the conception and the design of the manuscript and the collection, analysis and statistical interpretation of the data obtained. In addition, she was responsible for the design and the drafting of the article, as well as for reviewing it and preparing it for submission.
O-MJ participated in the conception and the design of the manuscript, the collection, analysis, and statistical interpretation of the data obtained. She was involved in the drafting of the article as well as in its critical review, making significant intellectual contributions. In addition, she gave her approval to the final version of the article and coordinated the work of the authorial team.
JL-I, HG-Y and ADV-C participated in the conception and the design of the manuscript and the collection and analysis of the data. They were also involved in the critical review of the article.
TS-J participated in the conception and the design of the manuscript, analysis of the data and developed the main statistical interpretation of the data obtained. He was also involved in the critical review of the article.
FLL-CM participated in the conception and the design of the manuscript, the collection, analysis, and statistical interpretation of the data obtained. She also participated in the drafting of the article as well as in its critical review, making significant intellectual contributions. She also gave her approval to the final version of the article.
Contributions| GC-B | O-MJ | JL-I | HG-Y | |
| Concept | YES | YES | YES | YES |
| Design | YES | YES | YES | YES |
| Definition of the intellectual content | YES | YES | YES | YES |
| Literature search | YES | YES | – | – |
| Clinical trials | – | – | – | – |
| Experimental studies | – | – | – | – |
| Data collection | YES | YES | YES | YES |
| Data analysis | YES | YES | – | – |
| Statistical analysis | YES | YES | – | – |
| Preparation of the manuscript | YES | YES | – | – |
| Editing of the manuscript | YES | YES | – | – |
| Review of the manuscript | YES | YES | YES | YES |
| Guarantor | YES | YES | YES | YES |
| ConceptDesign | ADV-CYESYES | TS-JYESYES | FLL-CMYESYES | |
| Definition of the intellectual content | YES | YES | YES | |
| Literature search | – | – | YES | |
| Clinical studies | – | – | – | |
| Experimental studies | – | – | – | |
| Data collection | YES | – | YES | |
| Data analysis | – | YES | YES | |
| Statistical analysis | – | YES | YES | |
| Preparation of the manuscript | – | – | YES | |
| Editing of the manuscript | – | YES | YES | |
| Review of the manuscript | YES | YES | YES | |
| Guarantor | YES | YES | YES |
All co-authors accept the responsibilities defined by the International Committee of Medical Journal Editors (available at http://www.icmje.org/).
In the event of publication, the authors exclusively transfer to the Revista and, by extension, to SEFH their rights to reproducing, distributing, translating, and publicly communicating their work by any sound, audiovisual or electronic medium or format. To that effect, a letter transferring such rights shall be attached to the paper when submitting it through the online manuscript management system.
FundingThis study has been carried out with the support of a grant provided by the Spanish Society of Hospital Pharmacists for the period 2015–2016.
Contribution to the scientific literaturePediatric patients have been identified as one of the population groups of highest risk of preventable harm from medications in all areas of patient care. Knowledge of the medication errors that occur most frequently among the pediatric population and an analysis of their causes is of primary importance and fundamental for establishing medication safety practices designed to minimize these errors in our healthcare settings.
Considering the types of errors detected and the underlying causes, strategies for medication error prevention in the pediatric population should be oriented fundamentally towards prescription methods, parents and/or caregivers for patients, and the general population.
We are grateful to all the professionals who contributed to the development of this project, and to the emergency services pediatricians and clinical pharmacists who gave of their time to assist with the initial sifting through of incidents.
Alcaraz Melgarejo MD, Garrido Sánchez MJ, Gutiérrez Sánchez E, Martínez García C, Rodríguez García J, Sánchez Castro M and Solano Navarro C (Virgen de la Arrixaca Clinical University Hospital, Murcia).
Alonso Martínez C, Cabañas Poy MJ, Cañete Ramírez C, Clemente Bautista S, Fernández Polo A, González Peris S, Rodrigo García R and Sancosmed Ron M (Vall d'Hebron University Hospital, Barcelona).
Fernández Elías M, Martínez Carapeto I, Moleón Ruíz M, Molero del Río MJ, Molina Mata M, Montecatine Alonso E, Núñez Pérez de Zafra M, Poyatos Ruíz LL, Quevedo García M, Rodríguez Lima MM, Rodríguez Martínez A, Romero Reina R, Sánchez Álvarez MJ, Sánchez Ganformina I, Sánchez Tatay V, Santos Rubio MD, Valero Flores NM and Villanueva Bueno C (Virgen del Rocío University Hospital, Sevilla).
Dolz Bui E, Fernández Ureña S and Otero Villalustre C (Maternal-Insular Hospital Complex of Gran Canaria, Gran Canaria).
García Cerezuela MD, Gumiel Baena I, Martos Sánchez I, Pérez García MJ, Repilado Álvarez A, Rodríguez Marrodán B and Sanz Rodríguez S (Puerta de Hierro University Hospital, Majadahonda, Madrid).
García García P, Gómez de Quero Masía P and Sánchez Moreno S (Salamanca University Hospital, Salamanca).
González Rodríguez I, Martín Prado S, Molina Cabañero JC and Pozas M (Niño Jesús University Pediatric Hospital, Madrid).
Lorente Romero J, Manrique Rodríguez S, Marañón Pardillo R, Míguez Navarro C, Mora Capín A, Rivas García A and Vázquez López P (Gregorio Marañón University General Hospital, Madrid).